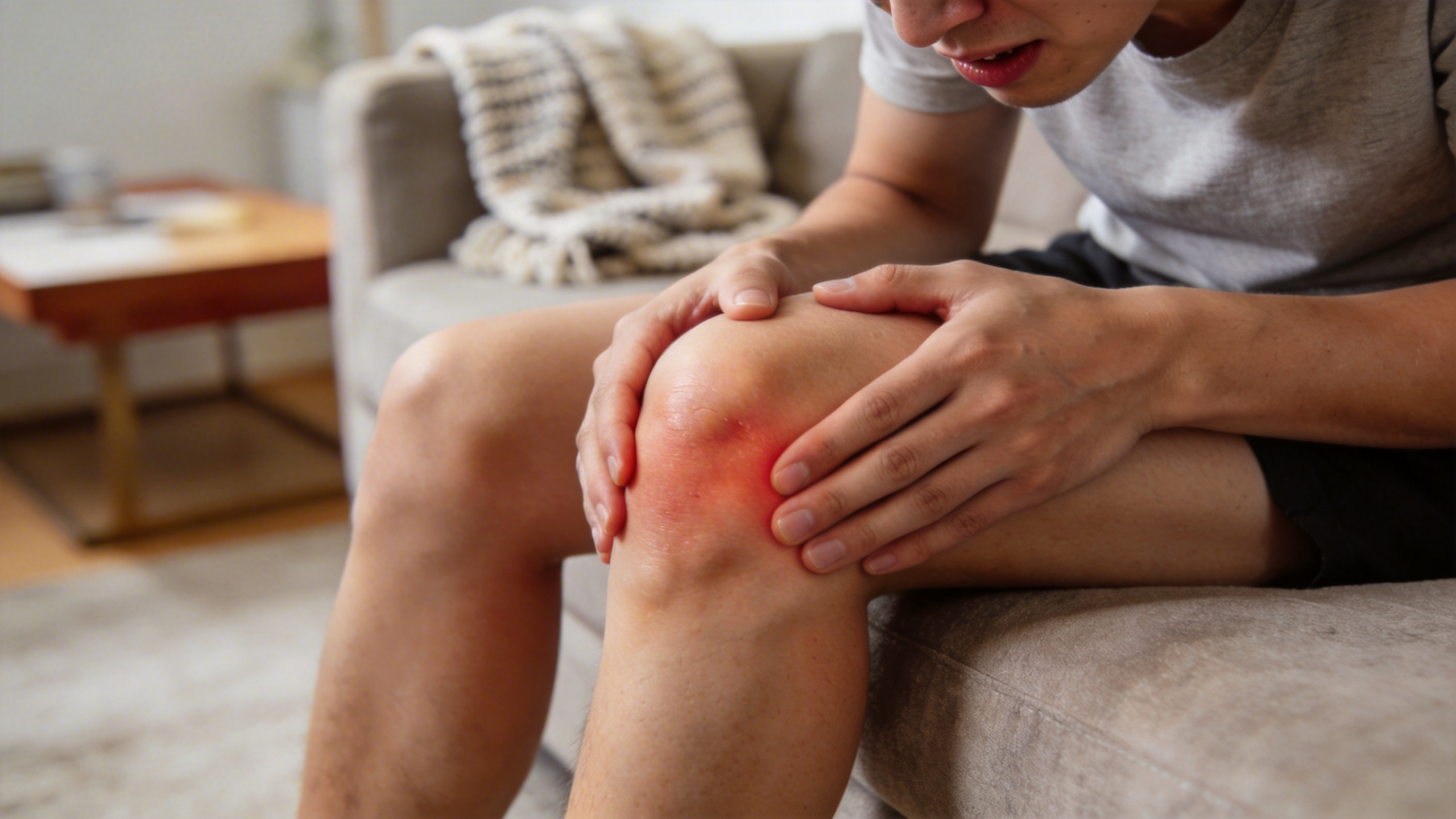
Millions of Americans suffer from knee pain secondary to arthritis. Knowing your options for how to best treat arthritis knee pain is key in helping to alleviate your pain and to prevent it from coming back.
Arthritis, also known as osteoarthritis (OA), is the degeneration of cartilage that helps our joints glide smoothly against each other. This cartilage can break down from trauma, autoimmune conditions, or wear and tear over time. The effects of this degeneration are what lead to the pain and sometimes swelling that we see in osteoarthritis.
So what are your best options for treating knee arthritis?
There are many options for treating knee OA that range from conservative to more invasive. Generally, most medical practitioners will start with the most conservative options and will get more aggressive with treating your OA pain as each successive option works less and less.
For this review, we will start with the least invasive options and continue on to more invasive options as we move forward.
1) Heat/Cold Therapy:
We have all used ice and or heat for one injury or another. The use of temperature to treat pain has been around for thousands of years. For those suffering from knee pain secondary to arthritis, this method is often overlooked. Studies have shown that using ice and/or heat can certainly relieve pain due to OA in the short term. If your pain is secondary to an acute flare-up, heat/cold therapy may be all you need.
There haven’t been any robust studies demonstrating how much and how often you can apply heat or ice to treat OA pain. When it comes to ice however the general rule of thumb is 30 minutes on and 30 minutes off. I would advise using a barrier material to prevent damage to your skin from the direct use of ice.
In regards to heat, there really is no limit as to how often you can use it. If it feels better with heat then you can use it liberally. If it doesn’t then you can stop using it. Just be sure not to leave a heating pad on overnight or while you are sleeping to prevent burn injuries.
2) Exercise:
Many studies have shown the benefits of exercise in helping to treat arthritis knee pain. The type of exercise and the duration will vary by individual. Whether it be physical therapy, leg strengthening, tai chi, or even swimming, the benefits of exercise cannot be ignored. Most people report some level of pain relief and improvement in function in the short term. Many studies show that if these exercises were part of a regular routine they would also result in an improvement in pain and function over the long term.
Not every modality of exercise will be beneficial to everyone. The type and duration of exercise must be tailored for you. What I recommend is that patients start by seeing a physical therapist or begin some low-impact activity (i.e. swimming, yoga, tai chi). As you progress through these activities for the first few weeks, keep in mind what works and what doesn’t. You should be able to complete the activity virtually pain-free. You also shouldn’t have any worsening in pain after the activity is completed.
By combining physical activity and a healthy diet, the hope is that you are not only making the muscles in your lower legs stronger but also losing any excess weight. Both leg strengthening and weight loss through exercise have been shown to contribute to pain relief from knee arthritis.
3) Knee Brace:
A knee brace is another often overlooked option for those suffering from knee pain secondary to arthritis. Specifically, the unloader knee brace has been clinically proven to decrease pain and increase functional mobility. They work by alleviating pressure in the area of your knee that has a loss in joint space from cartilage degeneration. They can be used daily to provide added support for your knee while also providing pain relief.
The unloader knee brace is custom-fitted to your type of arthritis and it may not be for everyone. Before getting one you should have imaging of your knee performed and speak to your doctor to know which type of unloader brace may be right for you. While some people complain of skin irritation from contact with the brace there are very few adverse effects from using an unloader knee brace.
4) Electrical Nerve Stimulation:
Transcutaneous electrical nerve stimulation (TENS) has been used to treat pain since the 1970s. While the evidence for its effectiveness in helping to treat arthritis knee pain has been mixed, it may still be worth trying. TENS works through a portable battery-operated device that delivers an electrical stimulation through the skin. This stimulation alters the sensation of pain that you notice at the central nervous system. The most serious side effects include local skin irritation, muscle soreness, and in very rare instances burn. You should always consult with your physician and ensure that you are using the proper machine settings before using a TENS apparatus.
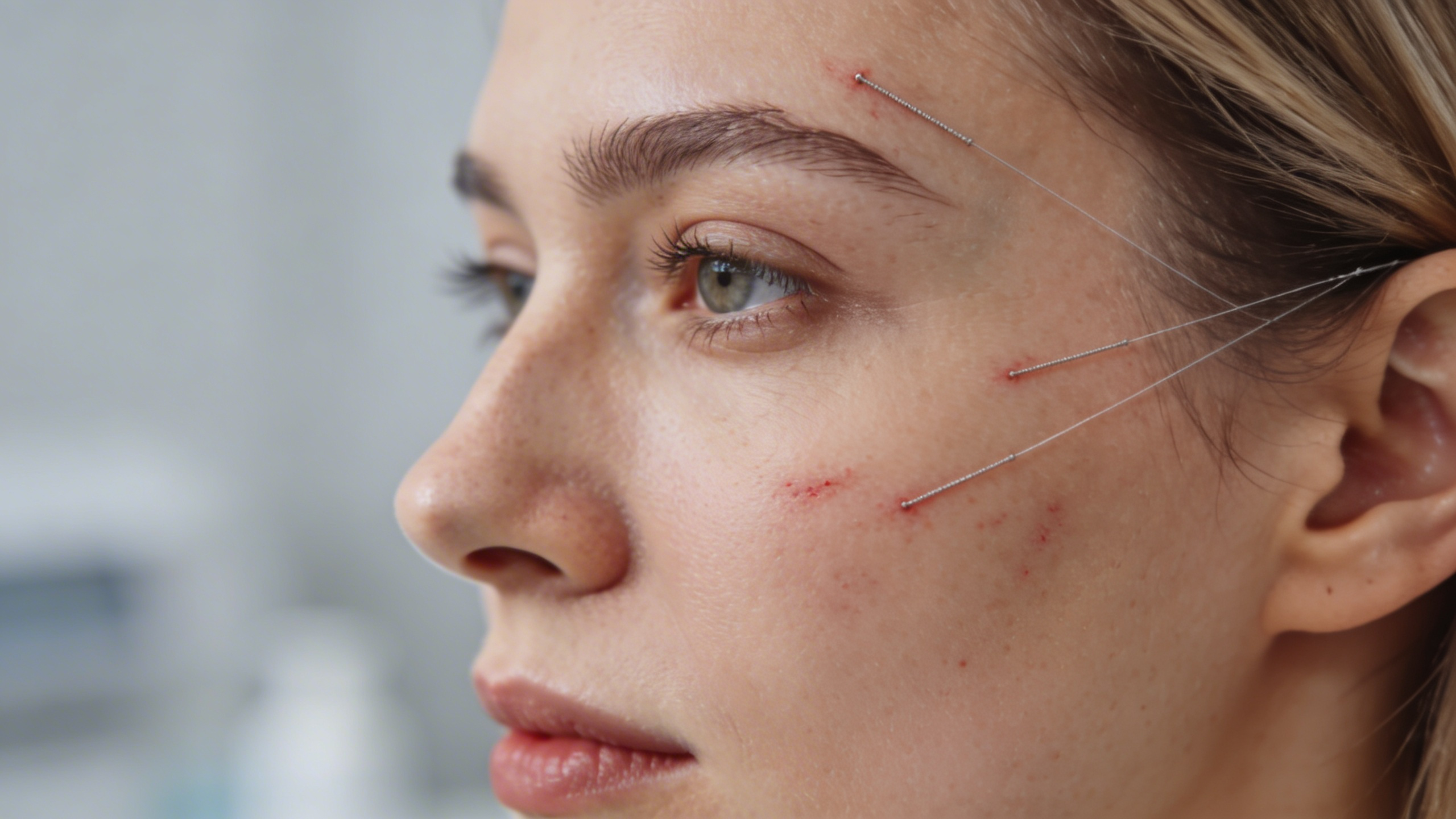
5) Acupuncture:
Evidence has been mixed to negative in regards to the effect of acupuncture in helping to treat arthritis knee pain. While acupuncture has been used for hundreds of years, there have been few scientific studies showing objective improvement in function with acupuncture. That being said, many people do experience a subjective improvement in pain. Before you decide to try acupuncture it’s important to make sure that the acupuncturist you use is certified to perform the procedure. They should also be using sterile equipment and technique to prevent infection. Acupuncture is commonly used in combination with the other modalities listed. If you are interested in learning more or even trying acupuncture contact our office for more information.
7) Topical Pain Medications:
There is strong evidence showing that topical medications can treat arthritis knee pain. In particular, topical Capsaicin or Menthol-based rubs (i.e. Bengay or Tigerbalm), as well as topical prescription anti-inflammatories (ie. Voltaren/Diclofenac gel), have been shown to improve knee pain. Capsaicin works as a counterirritant by directly causing a burning sensation at the skin. This modifies and can reduce the sensation of pain in the central nervous system when it is applied to a painful area.
Topical prescription antiinflammatories directly inhibit the pain signal locally. Because of the local effect of both of these topical medications, there is a low risk of systemic side effects. These options can be quite effective and their benefit can be enhanced when used with the other modalities discussed.
8) Supplements:
There are many supplement options for those with knee arthritis. Before trying any of these you should first understand that many of them may not work as well as you expect them too. Also, before starting any supplement you should always consult with your doctor.
Reviewing every supplement that has been used for knee arthritis would be beyond the scope of this article. However, a few supplements that have shown mixed to positive results include Fish-oil, Curcumin, Boswellia serrata extract, Glucosamine chondroitin, and Collagen hydrosylate. If you have any questions about which supplements might be right for you please contact our office.
9) Oral Pain Medications:
When it comes to oral pain medications for treating knee arthritis most doctors will prescribe either acetaminophen (Tylenol), non-steroidal antiinflammatories (i.e. Motrin, Aleve), or opioids (i.e. Oxycodone, Hydrocodone). All of these medications work by dulling signals along the neural pain pathway.
Studies have shown non-steroidal antiinflammatories (NSAIDS) to be most effective at treating arthritis pain. Acetaminophen is another great option as well. While studies show they may be inferior to NSAIDS, many patients who do not get relief from NSAIDS or cannot tolerate them, may find pain relief from acetaminophen.
Opioids are less commonly used for knee arthritis because of the high risk of addiction and the multitude of side effects. Your doctor may be more likely to use this as a short-term solution in the event that you will be having surgery. For those suffering from severe knee arthritis who may not be candidates for surgery, opioids may be a reasonable although less ideal option.
Before taking any of these medications it is important to speak with your doctor about the side effects. You also need to be honest about your medical history and medication/supplement use.
10) Corticosteroid Injections:
Steroid injections for knee pain can be an excellent option for those seeking short-term pain relief. Studies show that intra-articular steroids can provide improvement in pain and function for up to six weeks if not longer. When combined with other modalities, especially exercise, they can maximize pain relief and function.
These injections are only temporary and repeat injections have been shown to not be as effective. Multiple injections over time have been shown to actually increase joint degeneration and thus are not recommended.
Side effects from these injections can include worsening pain, bleeding, infection, localized skin irritation and in some instances skin discoloration. Make sure your provider is knowledgeable in how to perform this injection correctly to maximize the benefit you get from this procedure.
11) Hyaluronic Acid Injections:
Hyaluronic acid is a viscous polysaccharide found in connective tissue. Since the late 1990’s the FDA has approved Hyaluronic acid injections (more commonly known as gel injections or viscosupplementation) for the treatment of knee osteoarthritis. As of today, there are at least a dozen formulations on the market. While we aren’t 100% sure how they help with pain control, it is believed that they function by helping with joint viscosity. While more recent evidence has been mixed, evidence has shown that there is some improvement in both pain and function.
Your insurance will likely cover these injections and there is a very low risk of side effects when these injections are performed properly. Some uncommon side effects do however include increased pain, localized skin irritation, and infection. Make sure your provider is knowledgeable about how to perform these injections correctly to maximize the benefit you get from this procedure.
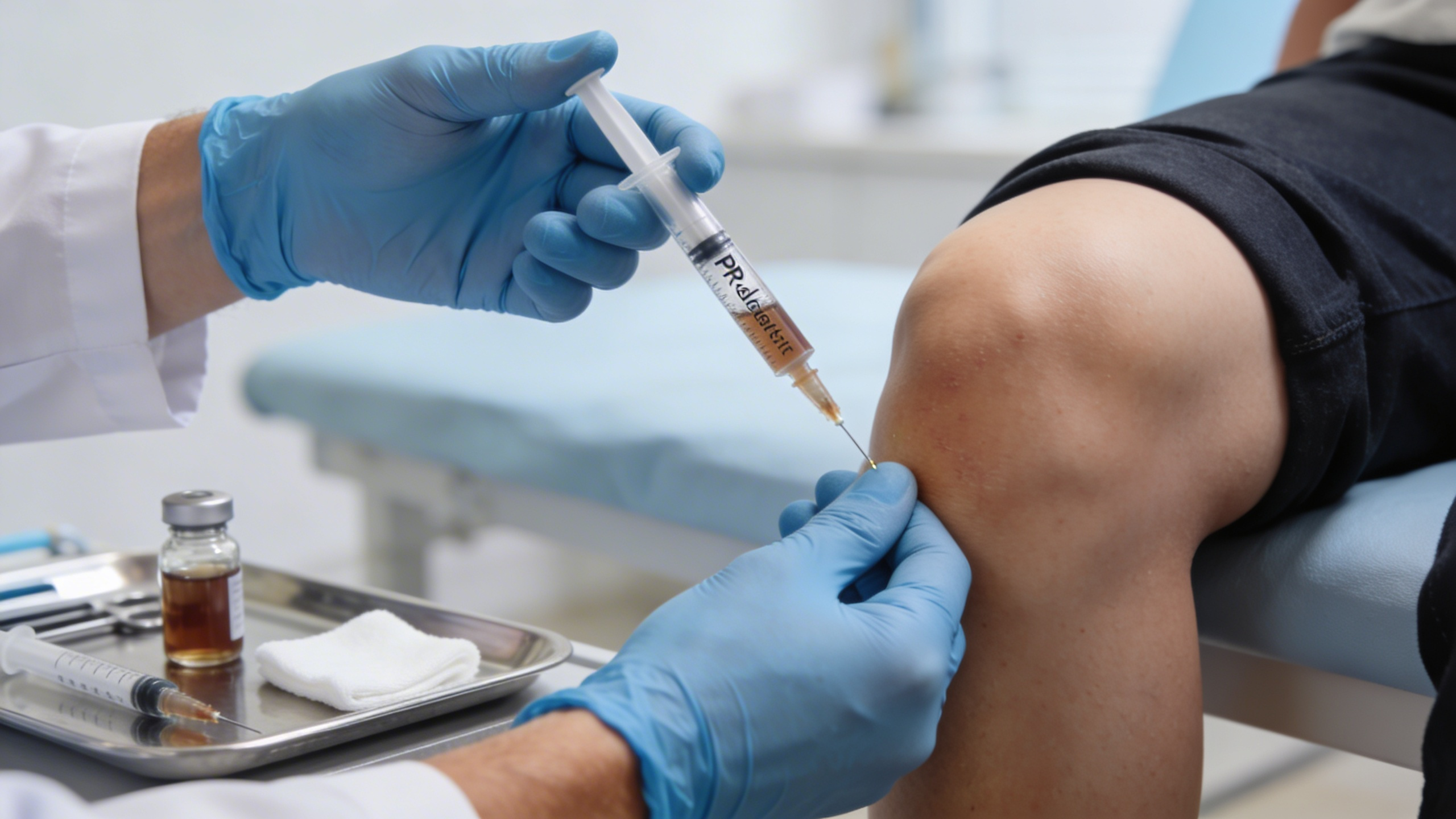
12) PRP injections:
Platelet-rich plasma (PRP) has traditionally been used for muscle and tendon injuries. More recent studies have shown some effectiveness in its ability to treat arthritis knee pain. PRP has been used for over 20 years and involves collecting your own blood and then separating out your body’s growth factors. This high concentration of growth factor can then be introduced into your knee joint. The theory behind this is that your joint will use these growth factors to begin the process of repairing some of the damaged cartilage. This may in turn help decrease your pain.
PRP has received FDA clearance but because of regulatory statutes it has not been labeled as FDA approved. Because PRP is not a drug and involves a person’s own blood product, it is not clearly subject to FDA approval. However, the devices used to collect and harvest PRP should be FDA-approved. No studies have shown a reversal in joint arthritis with PRP use. That being said, studies have shown an improvement in pain over time. Generally, the more severe your arthritis the less effective PRP injections may work. As of this writing, insurance does not cover these injections. Therefore, it’s important that you choose a provider with experience in performing them so that you can maximize their benefit.
13) Stem Cell injections:
The use of adult-derived stem cells to treat joint arthritis is part of a growing area of research. The FDA has not approved using your own adult stem cells or foreign stem cells for OA at this time. Any stem cell injection into your knee for OA is considered off-label and as of this writing is experimental.
The theory behind this injection is that once in your joint, these cells will communicate with your native tissue to begin the process of repairing the damaged cartilage that was lost. The regeneration of knee joint cartilage has only been seen in a few studies as it pertains to knee arthritis. However, studies do suggest that stem cells may alleviate arthritis pain. They may also alleviate your pain for a longer period of time than PRP or corticosteroid injections.
Despite the fact that early research has been promising, more high-quality studies need to be done to confirm whether or not stem cells improve cartilage degeneration from knee arthritis. Like PRP, stem cell injections are also not covered by your insurance. Side effects include increased pain, swelling, infection, and in rare instances tumor formation which has been seen when stem cells are injected into other parts of the body. If you are considering stem cell injections, finding a provider with expertise in both the harvesting and injection of stem cells will help to maximize your benefit and limit side effects from this procedure.
14) Surgery:
When all of the above options for knee arthritis have been exhausted then it is time to talk to an orthopedic surgeon about surgical options. Generally, the options for knee arthritis involve either knee replacement or some form of knee resurfacing. Debridement of the knee joint, where worn cartilage is either shaved down or removed, has for the most part fallen out of favor. However, It may still be an option for a very select group of patients.
If you find that you have tried all of your non-surgical options, then speaking to a surgeon who you trust may be the best option to help reduce your pain. I recommend seeing someone who both specializes in joint replacements and who has experience in replacement of knee joints in particular. For questions regarding surgeons we recommend here in Florida please contact our office.
Dr. Sergio Guiteau is a physician who has certifications in Aesthetic Medicine and is board certified in Family Practice and Sports Medicine. He specializes in Anti-Aging Medicine and blogs on rhm.sys.mybluehost.me/website_d5adaba3/blog